My Story: Part Four: Proton Beam Therapy
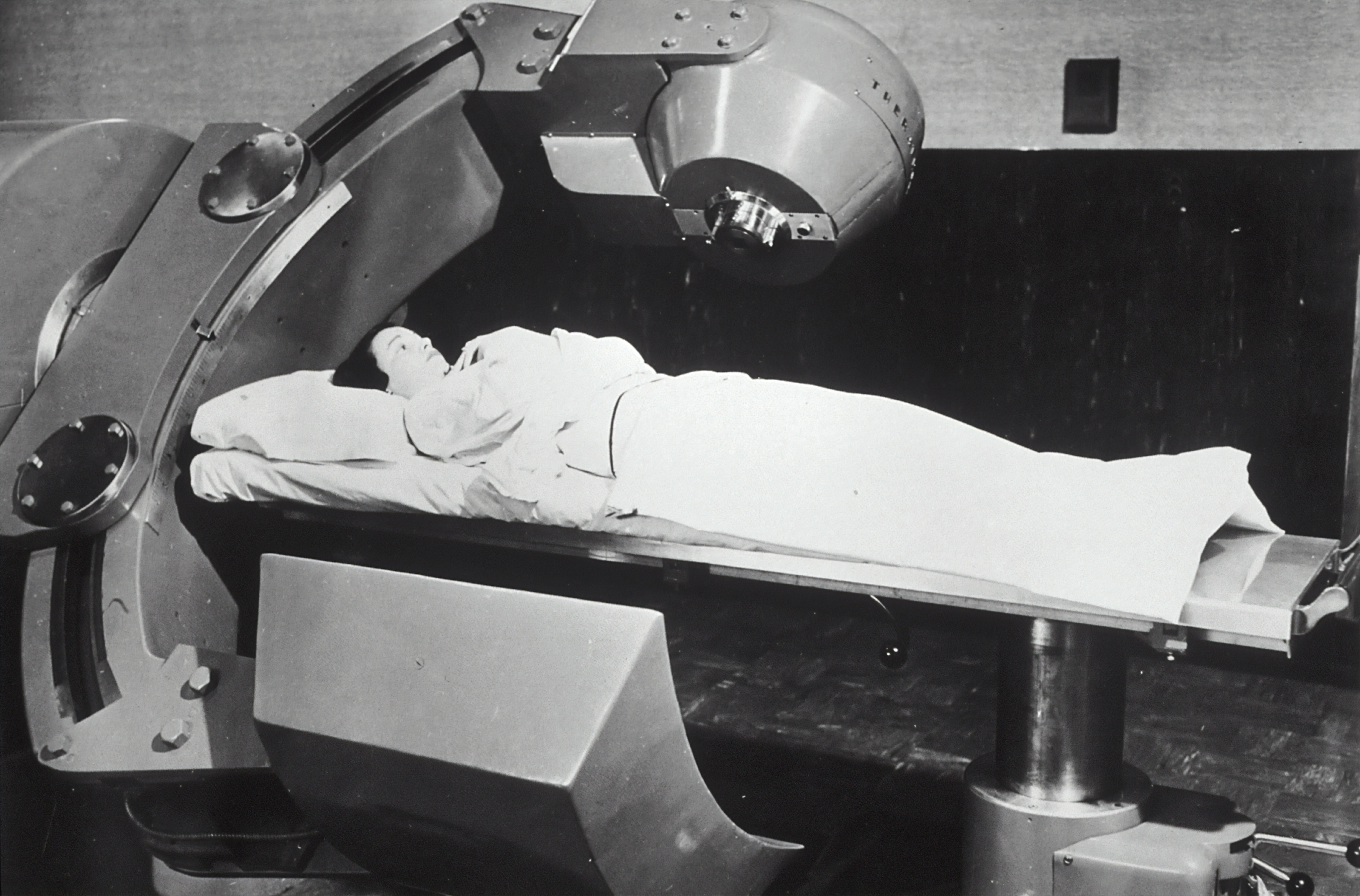
So in September of 2018, four months after my cancer diagnosis, I signed up for Proton Beam Therapy at California Protons Cancer Therapy Center with Dr. Urbanic, who initially recommended surgery, but agreed to treat me after I told him I refused surgery.
I immediately liked Dr. Urbanic, not because he was young, in his 40’s and also a surfer, but because I could tell he saw me as a person, not as my disease, medical record, or something to put on their resume.
When you have a rare cancer that most doctors have never treated before, doctors jump at the chance to treat you. I mean, not you personally, but your disease. They may refuse to refer you to the specialist because they want the case for themselves. They may even brag to their colleagues. “I got a Chordoma today.” Doctors never told me this, but I saw it in the way their eyes lit up. In the way they would often say, “Wow. A Chordoma!” As if I’m my disease, not a person.
One oncologist’s eyes lit up extra bright when he talked about the process of sawing off my sacrum with his new state-of-the-art machinery. “It’s not going to want to give, but I’m going to take that sucker down.”
Treatment Protocol
I would come in for eight weeks of Proton Beam Therapy, five days a week, Monday-Friday. I would be zapped with 77 grays, the dose of radiation. The typical radiation dose for cancer patients undergoing treatment hovers around 45 to 60 grays, but still, I had no idea what I was in for.
I was already in so much pain and by that time had switched from Percocet to morphine. There’s no way that my body could tolerate more pain. I was a 10 out of 10 whenever anyone asked, which was often. I was told that I might experience something like a bad sunburn on my skin and possibly some diarrhea.
The Pain and Side-effects
But by the fifth day of Proton Beam Therapy, I could no longer walk. Or sit. Or stand. When I sat, the pain was unbearable. I could only tolerate it for about twenty seconds. Standing caused all the nerves that ran up and down my legs to fire up. It was like being zapped or shocked endlessly, as if my nerves were going haywire. I could stand for only about 90 seconds.
I never had diarrhea, and the “sunburn” that was supposed to be the worst part was nothing compared to the internal bone pain and the nerve pain shooting up and down both legs. The bone pain felt as if someone had taken a bat and beat my sacrum repeatedly. The nerve pain felt like someone was slicing my nerves open with a sharp knife.
Unable to Walk, Stand, Sit
I remember trying to make myself a smoothie one morning. Once I made it to the kitchen, I put in the fruit and the protein powder and then would quickly go to the living room and lie down on the floor (always on my stomach) to alleviate the pain. After a few minutes, I would get up, put in the almond milk and sometimes the chia seeds too, if I could make it standing that long.
I usually had to lie down on the floor two or three times before I could finish making my smoothie. Mutsu found me lying on the floor crying, upset that I couldn’t do such a simple task for myself. So from that point, Mutsu started making my smoothies, and pretty much every meal. It would be several months before I could stand up long enough to make my own meals.
He also started witnessing me get out of bed in the morning, which was no easy feat. I felt like a 95-year-old woman as I wiggled my body in the perfect position to slowly dismount one toe at a time. With both feet planted on the ground I would slowly rise up to standing, grimacing in pain, one vertebrae at a time. There was nothing he could do to make it easier. That was the first of many times that I would see others’ heartache at the site of me, a once-athletic, once-vibrant, 35-year-old, suffering from so much physical pain.
I also remember not being able to stand up long enough to take a shower, but I couldn’t take a bath either because the skin above my sacrum was so badly burned. I ended up taking showers sitting on my knees. Awkward, I know. Also, awkward was getting to and from treatments in the car. I had to lay down on my stomach in the back. This was pretty much my position 23 hours a day: laying down on my stomach. Anything else was pure torture. I could sit on the back of my heels on the floor which I would do often for about 20-30 minutes of the time.
Quitting
By the time Monday came around, my second week of Proton Beam Therapy, I quit. I just couldn’t bring myself to get in the car and walk into another beating.
I sent Dr. Urbanic an email. I’m in too much pain, I wrote. Can’t make it. Won’t do it. Nope. Sorry. This is not right. After a few phone calls, he convinced me to come back by telling me he’d increase the pain meds and put me on steroids, and I reluctantly agreed. More morphine and now a strong steroid (6.0mg Dexamethasone). But it still took every ounce of strength to walk through those doors to the California Protons Center for each subsequent treatment. But I did it.
In October, about four weeks into my treatment, Mustu had to leave as his visa was about to expire, and I moved in with Mom and Dad. Around this time, the pain started getting worse. So I quit again. I told my mom, I’m not going. I’m not getting in the car. I then sent another email to Dr. Urbanic reiterating that I was in too much pain. I needed a break at least.

He called and called. Then a few other doctors started calling. I finally took his call. “We can hospitalize you if we need to, but we need to get you through the treatment. You can’t stop. You can’t take a break. I’m worried that if you stop this, there will be no other way to treat it.”
By then I had learned that surgery was out since most surgeons can’t operate on damaged post-radiation skin, especially with this high dose because the skin is so damaged that the wound won’t close. Having an open surgical wound, or a wound that won’t heal is an invitation to sepsis and subsequent death.
Increase in Pain Meds
So I succumbed and continued with the treatments. My morphine dose went up again, and by this time I was on 180mg of morphine each day. In total, I was taking 9 different pain medications. You can imagine how fuzzy my mind was at that time, so forgive me if I don’t remember all of them, but some of them were Flexeril, Gabapentin, Dexamethasone, Tramadol, Effexor, Cymbalta, and Dilaudid, another narcotic on top of the morphine. Most of these were at the max allowed dose.
Around that time, my mom came home from the pharmacy with something called Narcan. “What is that?” I asked. “In case you overdose,” she said. “The pharmacist and the pain management specialist thought we should have it on hand in case…”
That’s when I realized that by taking so many pain medications, I was risking my life. I’d learn later that this was normal for cancer patients. There’s a delicate balance, a fine line between relieving pain and risking death from overdose, or irreversible damage to the body, not to mention the potential addiction to opioids.
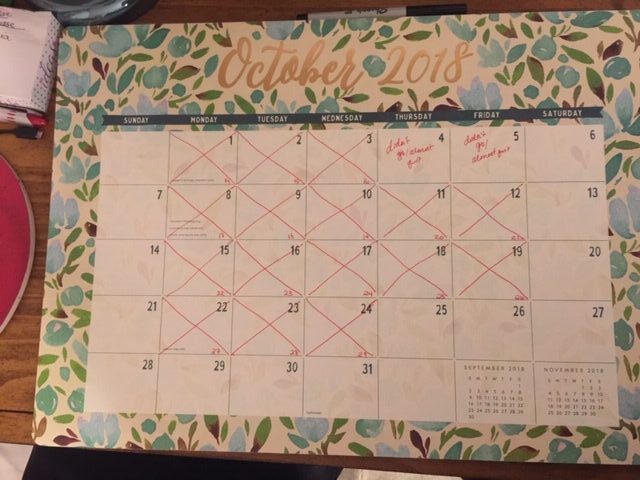
The eight weeks of proton beam therapy were blurry, to say the least. I used a walker to walk into my treatments. I couldn’t sit in the waiting room chairs, so the nurses would lead me back to an empty room where I would lay on a bed, waiting for my treatment session. Each day, I made a big red X on my calendar, counting down the days.
Deep Depression
At times, in so much pain, I prayed to not wake up in the morning. I often wondered if I should have just had the surgery because anything would be better than this. Now struggling with depression, I told God that if I could ever free myself of pain again, I would live my life to the fullest. I could have a good life if I were just out of pain.
At this point, I could deal with having cancer, with not being able to surf or walk again, but I could not deal with this level of physical pain. I wondered if I would ever be off of narcotics or whether I’d have to be on them for the rest of my life, like many other Chordoma patients I had met through a Facebook group.
Finally, after eight weeks, I completed the treatments. To celebrate the completion of the treatment, the staff (who was amazing and supportive) awarded me with a medal.

And the Tumor?
Every week I was having CT scans to check on the progress and every week Dr. Urbanic told me the same thing: it’s about the same size; it hasn’t shrunk. And each time, my heart sank. What I wanted so desperately to happen wasn’t happening.
Even worse, what I would find out later was that the tumor was actually still growing, little by little. Proton beam therapy had only slowed down the growth, not stopped it.
I could understand to some extent why he didn’t tell me it was still growing. The growth was probably too slight to see on a weekly basis. It also could have been inflammation, rather than actual growth. But one thing was for sure. By the end of my eight-week treatment, the tumor had not shrunk. I felt do defeated. But there was still hope that because radiation is cumulative, it could shrink in the coming months.
This was a very dark, dark time for me. I thought a lot about death. About my family. About what’s important and what’s not. My body was also overflowing with fear, depression and anxiety. Despite the darkness, I still held onto hope that it would shrink. My next MRI would be in three months, in February 2019. It had to get smaller, it just had to.









1 Response
[…] Continue to My Story: Part 4 […]